Periodontal Diseases
-“Perio” ~ around “dont” ~ tooth
-Periodontal disease is a bacterial infection of the gums and supporting tooth structures.
-This disease can occur at any place in the mouth
-Structures that surround each tooth include bone, ligament fibers, and the gums.
- Some infections can become so severe they cause permanent damage structures around the teeth
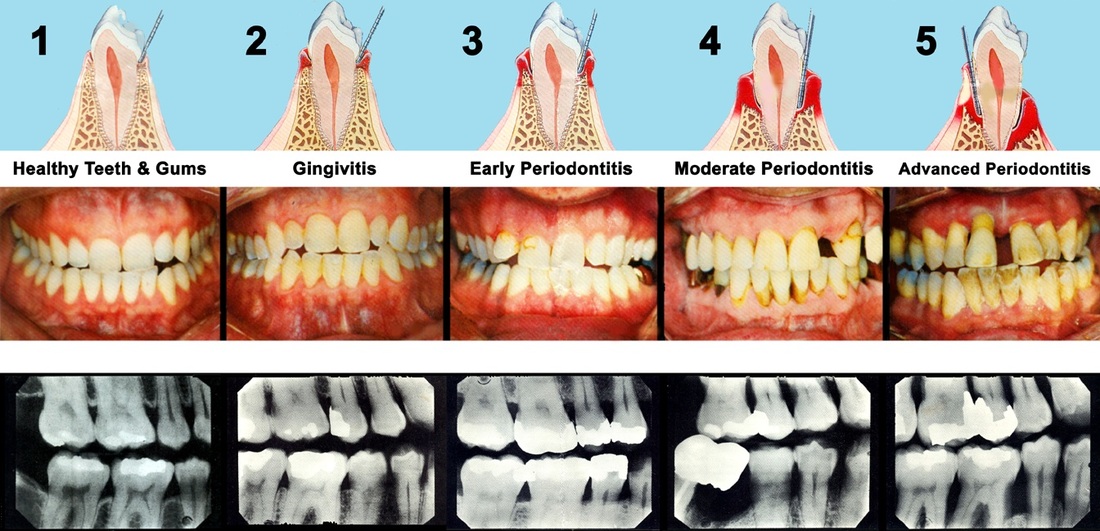
- The two types of periodontal disease include: Gingivitis and Periodontitis
What’s REALLY happening when my gums swell?
Inflammation seen and felt, is accompanied by the damage of underlying tissue. The damage is the result of your own body’s immune system. The body is trying to destroy invading pathogenic bacteria (bacteria that are capable of causing disease) by sending lots of bacteria killing cells, also known as white blood cells (WBC). Some of the most common WBC’s used by your body’s immune system, to protect you are polymorphonuclear leukocytes (PMN), monocytes/ macrophages, B-cells, T-cells, and fibroblasts.
When pathogenic bacteria make their way to the tooth and travel down into the space between the gums and teeth, PMN’s are the first cells of the immune system that will arrive. PMN’s using chemicals, try their best to destroy these pathogenic bacteria.
At this point, the PMN’s are either 1. Successful at eliminating these disease causing bacteria or 2. They are unsuccessful, resulting in gingivitis or inflammation of the gingiva “gums.” The body responds by sending more PMN’s, macrophages and T-cells, all which will release their own toxic chemicals. These chemicals are intended to kill pathogenic bacteria, but inadvertently damage gum tissue.
If these additional WBC’s can’t destroy these bacteria, the bacteria will travels underneath the gum tissues and begin to disrupt the gums that are physically attached to the tooth. Gingivitis is now established. B-cells, plasma cells, and fibroblasts head towards the pathogenic bacteria.
Pathogenic bacteria, if not eliminated, will continue to travels towards the root of the tooth, the periodontitis develops. The toxins being released by WBC’s will continue to destroy everything around them, like the supporting structures of the tooth. When the bone, periodontal ligaments (PDL), cementum, and gums are destroyed they are permanently damaged.
Gingivitis or Periodontitis?
Gingivitis ~ a bacterial infection confined to the gums.
Causes of gingivitis
-plaque
-bacterial infections
-viral infections
-genetic conditions
-trauma
How your gums might appear to you
-pink to red in color
-shiny and swollen
-uneven boarders when you gums meet the teeth
-bleeding during brushing &flossing
What your dentist & hygienist will see on your x-rays
-NO sign of bone loss
* If this disease is caught within its early stages, it can be reversible with proper oral home care. The mouth has the ability to return to a normal, healthy state.
Periodontitis ~ a bacterial infection involving the bone around the teeth, the ligaments attaching them, the gums supporting them, and the cementum layer over their root surface.
Causes of Periodontitis
-large amounts of harmful bacteria in the mouth
- the immune response to these bacteria causes destruction
How your gums might appear to you
- pink to purplish in color
-swollen
-possible bleeding
-firm and leathery consistency
What your dentist & hygienist will see on your x-rays
-PERMANENT bone loss
* Bone loss is a permanent and irreversible condition found with periodontitis. This infection needs to be arrested to limit the chance of the infection persisting to the chronic stage.
Chronic periodontitis~ the most common type of periodontitis, is a bacterial infection with chronic inflammation of the teeth's supporting tissues, damage to the ligaments, and destruction of bone. Usually seen in adults over the age of 35, but can occur at any age.
How your gums might appear or feel to you
-red
-swollen
-bleeding when brushing
-loose or sensitive teeth
-pus
- bad taste in mouth or breath
-jaw pain
*Little or no pain may be associated with this type of periodontal disease.
What your dentist & hygienist will see on your x-rays
-PERMANENT bone loss
**You CAN NOT determine what type of periodontal disease you have by what you see when you look at your gums, but if you see any of these signs or experience symptoms you should contact your dental care team as soon as possible for treatment.
** It is very important that your dental care team have a current set of X-rays. It is our tool to see what is happening under the gums
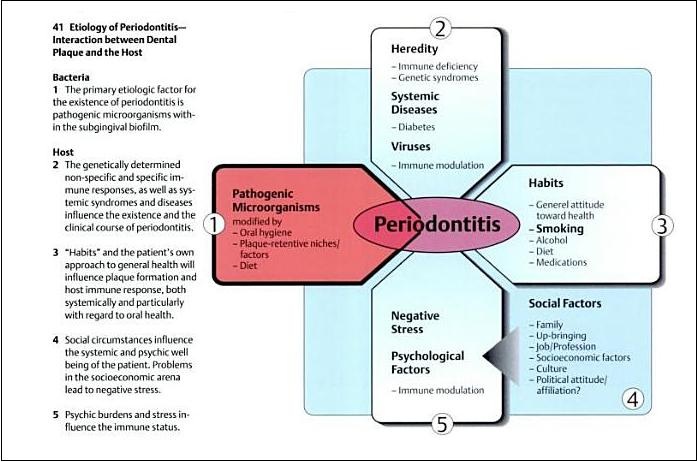
Local Contributing Factors that could increase your risk of Gum Disease
-Plaque buildup
-Calculus
-Tooth morphology (shape, pits, and grooves)
-Impacted food
-Forces on teeth from clenching and grinding
* Local contributing factors do not initiate periodontal disease, but can influence the progression of disease
Systemic Factors that could increase your risk of Gum Disease
-HIV/AIDS
-Leukemia
-Diabetes mellitus
-Genetics
-Hormonal changes (puberty, pregnancy, and menopause)
-Tobacco use
-Certain Medications
*Systemic factors can increase a persons susceptibility to developing periodontal disease
Frequently asked Questions..........
How do I know which type of Periodontal Disease I have?
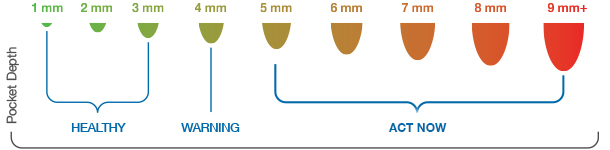
Unlike periodontitits, there is no attachment loss with gingivitis. Attachment loss is measured using a periodontal probe. The probe is inserted to the space between your gums and teeth (the sulcus or pocket) and moved along all sides of the tooth to record attachment loss. Your hygienist will record these numbers and determine which stage of periodontal disease you are currently at. Early stages of periodontal disease, like gingivitis, is reversible with proper oral health care.
Inflammation seen and felt, is accompanied by the damage of underlying tissue. The damage is the result of your own body’s immune system. The body is trying to destroy invading pathogenic bacteria (bacteria that are capable of causing disease) by sending lots of bacteria killing cells, also known as white blood cells (WBC). Some of the most common WBC’s used by your body’s immune system, to protect you are polymorphonuclear leukocytes (PMN), monocytes/ macrophages, B-cells, T-cells, and fibroblasts.
When pathogenic bacteria make their way to the tooth and travel down into the space between the gums and teeth, PMN’s are the first cells of the immune system that will arrive. PMN’s using chemicals, try their best to destroy these pathogenic bacteria.
At this point, the PMN’s are either 1. Successful at eliminating these disease causing bacteria or 2. They are unsuccessful, resulting in gingivitis or inflammation of the gingiva “gums.” The body responds by sending more PMN’s, macrophages and T-cells, all which will release their own toxic chemicals. These chemicals are intended to kill pathogenic bacteria, but inadvertently damage gum tissue.
If these additional WBC’s can’t destroy these bacteria, the bacteria will travels underneath the gum tissues and begin to disrupt the gums that are physically attached to the tooth. Gingivitis is now established. B-cells, plasma cells, and fibroblasts head towards the pathogenic bacteria.
Pathogenic bacteria, if not eliminated, will continue to travels towards the root of the tooth, the periodontitis develops. The toxins being released by WBC’s will continue to destroy everything around them, like the supporting structures of the tooth. When the bone, periodontal ligaments (PDL), cementum, and gums are destroyed they are permanently damaged.
Gingivitis or Periodontitis?
Gingivitis ~ a bacterial infection confined to the gums.
Causes of gingivitis
-plaque
-bacterial infections
-viral infections
-genetic conditions
-trauma
How your gums might appear to you
-pink to red in color
-shiny and swollen
-uneven boarders when you gums meet the teeth
-bleeding during brushing &flossing
What your dentist & hygienist will see on your x-rays
-NO sign of bone loss
* If this disease is caught within its early stages, it can be reversible with proper oral home care. The mouth has the ability to return to a normal, healthy state.
Periodontitis ~ a bacterial infection involving the bone around the teeth, the ligaments attaching them, the gums supporting them, and the cementum layer over their root surface.
Causes of Periodontitis
-large amounts of harmful bacteria in the mouth
- the immune response to these bacteria causes destruction
How your gums might appear to you
- pink to purplish in color
-swollen
-possible bleeding
-firm and leathery consistency
What your dentist & hygienist will see on your x-rays
-PERMANENT bone loss
* Bone loss is a permanent and irreversible condition found with periodontitis. This infection needs to be arrested to limit the chance of the infection persisting to the chronic stage.
Chronic periodontitis~ the most common type of periodontitis, is a bacterial infection with chronic inflammation of the teeth's supporting tissues, damage to the ligaments, and destruction of bone. Usually seen in adults over the age of 35, but can occur at any age.
How your gums might appear or feel to you
-red
-swollen
-bleeding when brushing
-loose or sensitive teeth
-pus
- bad taste in mouth or breath
-jaw pain
*Little or no pain may be associated with this type of periodontal disease.
What your dentist & hygienist will see on your x-rays
-PERMANENT bone loss
**You CAN NOT determine what type of periodontal disease you have by what you see when you look at your gums, but if you see any of these signs or experience symptoms you should contact your dental care team as soon as possible for treatment.
** It is very important that your dental care team have a current set of X-rays. It is our tool to see what is happening under the gums
Local Contributing Factors that could increase your risk of Gum Disease
-Plaque buildup
-Calculus
-Tooth morphology (shape, pits, and grooves)
-Impacted food
-Forces on teeth from clenching and grinding
* Local contributing factors do not initiate periodontal disease, but can influence the progression of disease
Systemic Factors that could increase your risk of Gum Disease
-HIV/AIDS
-Leukemia
-Diabetes mellitus
-Genetics
-Hormonal changes (puberty, pregnancy, and menopause)
-Tobacco use
-Certain Medications
*Systemic factors can increase a persons susceptibility to developing periodontal disease
Frequently asked Questions..........
How do I know which type of Periodontal Disease I have?
Unlike periodontitits, there is no attachment loss with gingivitis. Attachment loss is measured using a periodontal probe. The probe is inserted to the space between your gums and teeth (the sulcus or pocket) and moved along all sides of the tooth to record attachment loss. Your hygienist will record these numbers and determine which stage of periodontal disease you are currently at. Early stages of periodontal disease, like gingivitis, is reversible with proper oral health care.
Can I reverse Periodontitis?
Unfortunately, periodontitis is not reversible. However, you can arrest periodontitis and stop the bone and attachment loss. If you have been diagnosed with periodontitis, permanent damage has been done to any or all of the structures that surround the tooth; bone, PDL, cementum, or gums. Discuss your options your with hygienist, set a goal to arrest your periodontitis and preserve the health of your teeth and the structures around them.
I know I have signs of gingivitis, how long do I have until my gingivitis becomes periodontitis?
Gingivitis does not always progress to periodontitis. There is no set timeline, if you do have gingivitis you should work with your hygienist to develop the best home care routine for you. With proper oral home care, gingivitis can be reversible.
Nield-Gehrig,J. (2011). Foundations of periodontics for the dentils hygienist. (3 Ed.). Philadelphia: Lippincott Williams & Wilkins.
Image retrieved from: OraPharma, I. (n.d.). Retrieved from http://www.arestin.com/periodontal-gum-disease/stages.php
Image retrieved from http://bohone09.wikispaces.com/file/view/Periodontitis.jpg/92324994/Periodontitis.jpgcom/Periodontal_Images.png
Image retrieved from: OraPharma, I. (n.d.). Retrieved from http://www.arestin.com/periodontal-gum-disease/stages.php
Image retrieved from http://bohone09.wikispaces.com/file/view/Periodontitis.jpg/92324994/Periodontitis.jpgcom/Periodontal_Images.png